AARP Hearing Center
Mammogram Study: Are We Missing the Point?
By Candy Sagon, February 14, 2014 04:33 PM
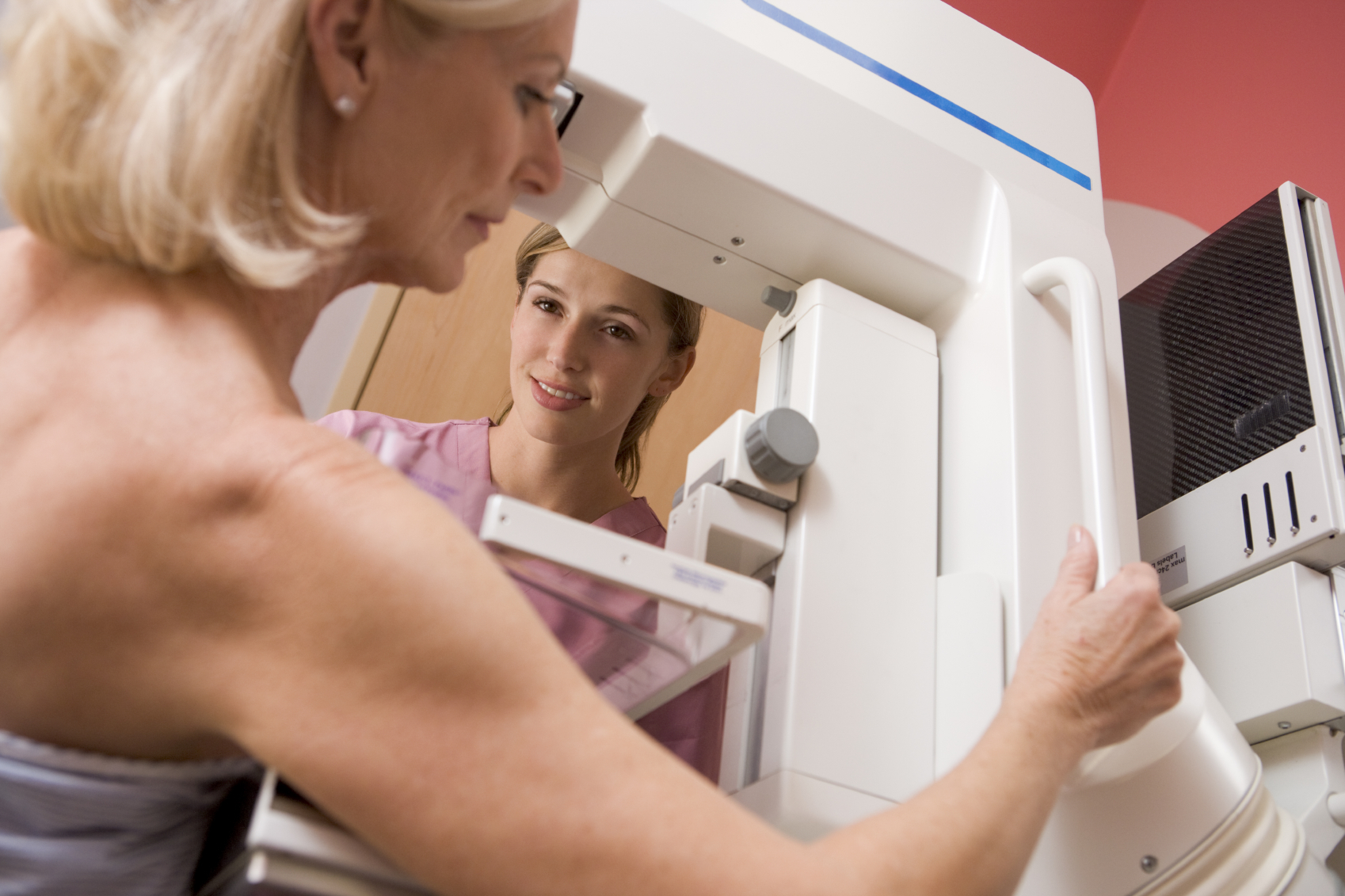
It's a large, new study that raises doubts about the value of mammograms in preventing breast cancer deaths, but a lot of the publicity and debate about it seems to have missed an important point.
According to the 25-year Canadian study, published Tuesday in BMJ (formerly the British Medical Journal), there was no difference in the number of breast cancer deaths between women who got annual mammograms and women who got an annual physical breast exam by a nurse.
The approximately 90,000 women ages 40 to 59 were randomly assigned to one of the two groups and followed for 25 years. In each group, slightly more than 3,000 women were diagnosed with breast cancer. Of those, 500 women died from breast cancer in the mammo group, and 505 died in the exam-only group.
But here's what didn't get mentioned in most of the news coverage: The study also showed that a significantly larger percentage of the women in the mammogram group lived for 25 years after their diagnosis than did the women in the exam-only group.
>> Sign up for the AARP Health Newsletter
In addition, the researchers found that a woman's chances of living those 25 years post-diagnosis were even greater if her mammogram detected a tumor that was "non-palpable" - meaning it couldn't be felt during a physical exam.
Women in the study had a nearly 80 percent chance of surviving another 25 years if their mammogram found a tiny, non-palpable tumor, versus a 66 percent chance if it was a larger, palpable one. Women who had a lump that was large enough to be felt during a physical exam had only a 63 percent chance of surviving 25 years.
Adding to the argument of finding tumors early was the researchers' finding that overall, "the 25-year survival was 77.1 percent for women with tumors of less than 2 cm [less than an inch], compared with 54.7 percent for tumors greater than 2 cm."
"Mammography has its disadvantages," acknowledges Carol Lee, M.D., a radiologist at Memorial Sloan Kettering Cancer Center in New York, "but it still remains the best way to find cancers, and clearly we are more successful at treating small, localized cancers than larger ones that have spread."
Lee called the publicity the study has generated "frustrating," because she worries that it will "discourage women from getting a mammogram and reverse the gains we've worked so hard to achieve."
"There are six or seven other randomized, large studies that have shown a benefit for screening," she said in an interview. "This one is an outlier."
The new study did find that mammograms overdiagnosed one in every 424 women, detecting what seemed to be an invasive cancer when it really wasn't. This, critics say, can lead to overtreatment for conditions that never would have threatened a woman's health.
An editorial accompanying the study, titled "Too Much Mammography," contended that better treatments, like tamoxifen, have lessened the importance of finding breast cancer early and are the reason breast cancer deaths have been decreasing.
>> Get discounts on health services with your AARP Member Advantages.
The authors argued that mammograms were similar to the prostate-specific-antigen (PSA) testing for prostate cancer in both their overdiagnosis rate and their small effect in lowering cancer deaths.
But Lee disagrees with the conclusion that overdiagnosis is leading to tiny harmless tumors being overtreated: "We don't know which tumors are potentially lethal and which aren't. Should we wait until they get big enough to be palpable? No rational person would think that's a reasonable thing to do."
The answer, she says, "isn't to stop finding all cancers; the answer is to find better molecular markers to figure out which ones are dangerous."
Currently, guidelines differ on how often a woman needs a mammogram. The American Cancer Society supports an annual one starting at age 40; other expert panels say women in their 50s and 60s need only one every two years. And, of course, women at high risk because of family history, obesity, smoking and other factors need to discuss their personal situation with their doctors to determine the best course.
Some of the confusion might be resolved later this year when the American Cancer Society, which is reviewing all mammography studies including this one, issues new guidelines.
Photo: monkeybusinessimages/iStock
Also of Interest
- Eye Infection Sidelines Bob Costas at Olympics
- 6 Fabulous Foods to Fight High Blood Pressure
- Get free assistance with tax-return preparation from Tax-Aide
- Join AARP: Savings, resources and news for your well-being
See the AARP home page for deals, savings tips, trivia and more































































