AARP Eye Center
Is Observation Status Substituting for Hospital Readmission?
By Claire Noel-Miller, Keith Lind, November 13, 2015 11:51 AM
Since October 2012, the Medicare program has penalized hospitals when too many patients in traditional Medicare are re-hospitalized within a month of discharge. This policy appears to be having unintended consequences for patients in Medicare and in the commercial market.
Hospitals with readmission rates above the national average now receive lower payments across-the-board from Medicare; the higher the rate of “excess” readmissions, the greater the penalty. The fines are intended to push hospitals to provide better care for their patients both in and out of the hospital to avoid having patients return.
However, when patients do return to the hospital, the policy may unintentionally encourage hospitals to keep them “under observation” to circumvent the penalties. A patient “under observation” is in outpatient status and not admitted to the hospital. A subtle difference, but one that may have significant financial consequences for some patients — treatment under observation could mean denial of coverage for necessary follow-up care in a nursing home, and huge medical bills.
For example, patients under observation can end up owing thousands of dollars for follow-up care in a skilled nursing facility, as we described in another paper. Why? Because Medicare requires that beneficiaries have at least three inpatient hospital nights before covering such care.
There are possible indications that in the new world of readmission penalties, some clinicians are placing more returning Medicare patients under observation. Our independent analysis of Medicare data published by the Centers for Medicare & Medicaid Services (CMS) revealed that the top 10 percent of hospitals with the largest drop (16 percent on average) in readmission rates between 2011 and 2012 also increased their use of observation status for Medicare patients returning within 30 days by an average 25 percent over the same time period (figure 1).
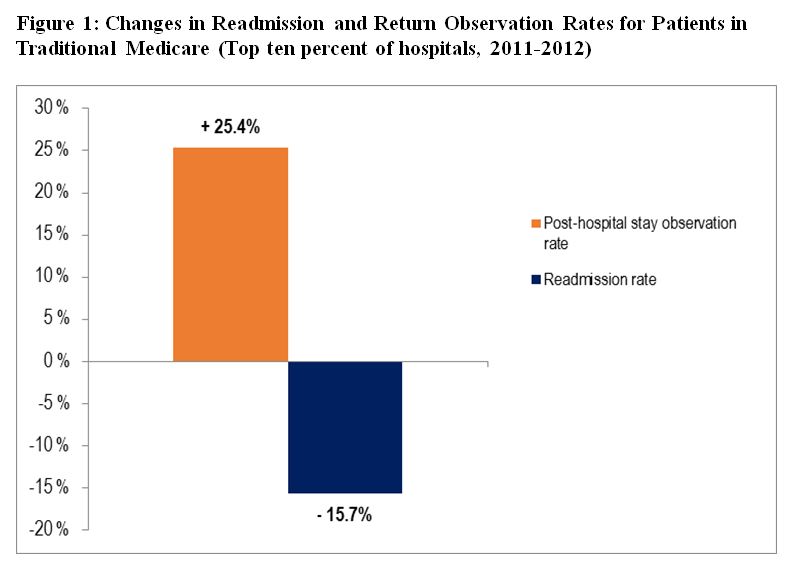
The policy also appears to be affecting commercially insured patients. Patients not covered under Medicare do not affect a hospital’s readmission penalties. But Medicare, as the country’s largest payer for health care services, often influences how hospitals care for all patients. Using data from the OptumLabs™ Data Warehouse, which includes claims from a large health insurance carrier, we found that hospitals that reduced readmissions within 30 days also increased their share of returning observation patients in private plans. The top third of hospitals with the largest six-year (2009-2014) reduction in 30-day readmissions (26 percent on average) increased their share of returning observation patients by an average of 45 percent (figure 2)[1]. Much of that increase started in 2012, the same year that Medicare hospital readmission penalties began.
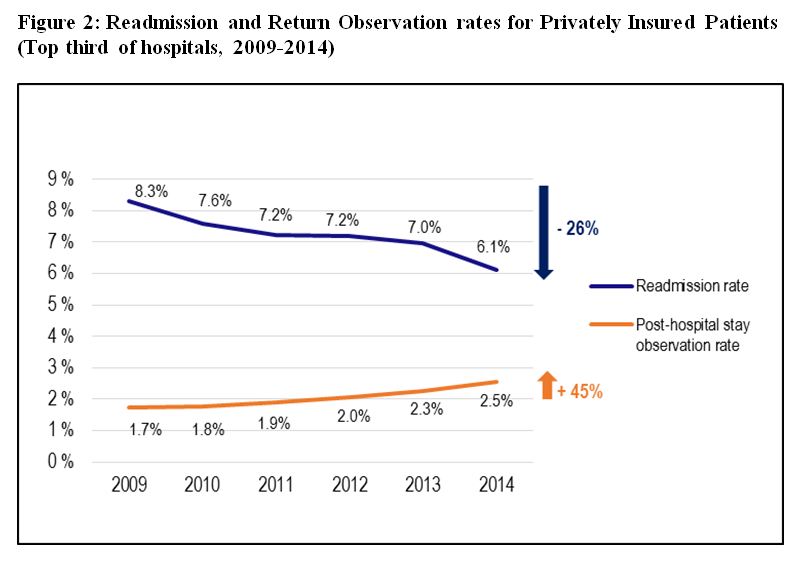
This association between observation status and readmissions raises a number of questions. For instance, do observation patients get the same quality of care as inpatients? Further, are privately insured observation status patients spending more on subsequent health care, as are some Medicare beneficiaries? A forthcoming report will examine the financial and health outcomes of privately insured patients under observation.
[1] These findings apply to the health insurance carrier’s enrolled population and are not necessarily representative of the U.S. population.
NOTE: This blog was originally posted on the Health Affairs blog.

Claire Noel-Miller is a senior strategic policy adviser for the AARP Public Policy Institute, where she provides expertise in quantitative research methods applied to a variety of health policy issues related to older adults.

Keith Lind is a senior policy adviser for the AARP Public Policy Institute, where he covers issues related to Medicare post-acute care and chronic care.
Also of Interest
- New Medicare program may be reducing hospital readmissions for joint replacement patients
- Downsizing? Ditch these 12 items
- Get Help: Find out if you're eligible for public benefits with Benefits QuickLINK
- Join AARP: savings, resources and news for your well-being
See the AARP home page for deals, savings tips, trivia and more.























































