AARP Hearing Center
Stability Fund Won’t Keep Premiums From Going Through the Roof for People With Preexisting Conditions
By Lina Walker, Claire Noel-Miller, Lynda Flowers, and Jane Sung, May 25, 2017 11:59 AM

The American Health Care Act (AHCA), H.R.1628, allows states to create high-risk pools for people with preexisting health conditions under certain circumstances. High-risk pools are supposed to provide access to health insurance for people who cannot get coverage in the individual (non-group) health insurance market. In a previous analysis, we noted that states have never funded high-risk pools adequately. The result: A small number of consumers paid very high premiums for skimpy coverage. Many others went without health insurance because they could not afford it.
What was true then is still the case today. Yesterday, the Congressional Budget Office (CBO) released its analysis of the AHCA. It projected that in states with high-risk pools where insurers can charge consumers higher premiums based on their health, “ over time, less healthy individuals (including those with preexisting or newly acquired medical conditions) would be unable to purchase comprehensive coverage with premiums close to those under current law and might not be able to purchase coverage at all.”
In this blog, we illustrate the impact on consumer premiums if states choose to go this route in 2019 — when the AHCA would allow health insurers to consider people’s health when deciding how much to charge them. If consumers have to buy coverage in high-risk pools that is comparable to that available under current law, we estimate that they could face average premiums of at least $25,000. Premiums would vary by state, ranging from at least $19,330 in Iowa to over $38,600 in Alaska in 2019 .
The AHCA would create the Patient and State Stability Fund (Stability Fund): $15 billion in 2018 and 2019, and $10 billion each year for the following eight years, to — among other things — establish state high-risk pools. States could use these dollars to help offset consumer premiums in the high-risk pools. To illustrate the inadequacy of these funds, our estimates assume that states would use their entire Stability Fund allotment to reduce premiums for people in high-risk pools. The bill also includes an extra $8 billion over five years (an average of $1.6 billion for each year) for state high-risk pools. We assume that states would also apply all of these funds to reduce high-risk pool premiums.¹ Despite these offsets, premiums would remain astonishingly high.
The funding levels in the AHCA are a drop in the bucket: The Stability Fund would not shield consumers from unbearable premiums. We need policies that ensure access to affordable coverage for everyone.
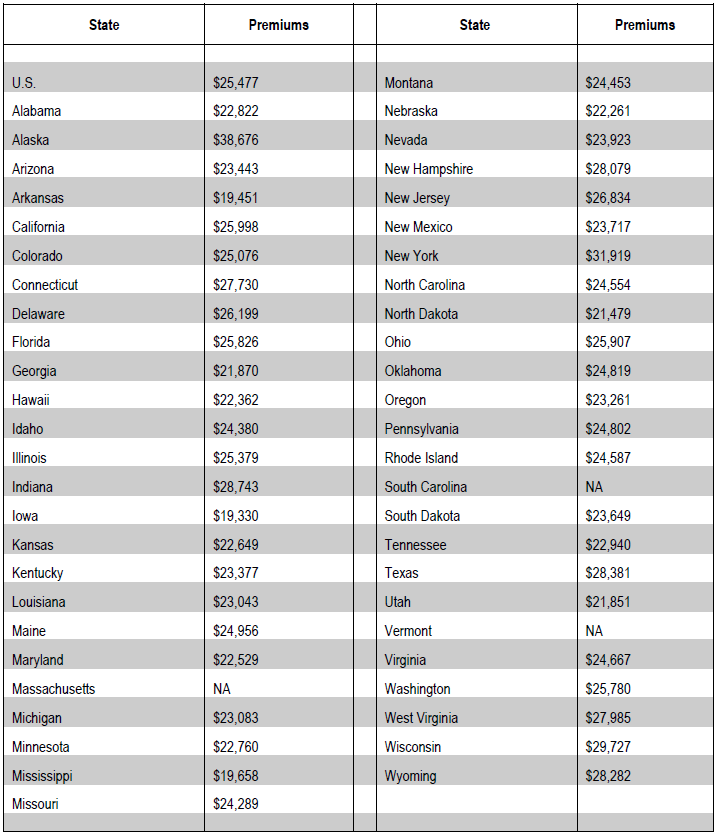
Source: AARP Public Policy Institute
Notes:
We were not able to derive premium estimates for Massachusetts, Vermont and South Carolina because the data for these states were not available.
It is unlikely that all states will seek a federal waiver to use health status as a factor in developing premiums. Seven states (Maine, Massachusetts, New Jersey, New York, Oregon, Vermont and Washington) did not allow insurance companies to charge higher premiums based on health status before the Affordable Care Act (ACA). Therefore, these states are unlikely to seek a federal waiver under the AHCA to allow this practice.
We thank Michael Chernew and the team at the Health Care Markets and Regulation Lab at Harvard Medical School for support with this analysis.
Methodology
Health insurance premiums reflect the expected health insurance benefit payout plus an administrative load, which we assume to be 20 percent, consistent with the medical loss ratio under current law. The typical plan in the individual market is the silver plan, with an actuarial value (AV) of 70 percent. We therefore constructed premiums for a 70 percent AV plan to reflect what consumers would pay if they wanted to buy the same coverage in 2019 — when the AHCA allows insurers to use medical underwriting under certain circumstances.
We estimated the top 10 percent of adults (ages 18-64) with the highest risk of using state high-risk pools and computed spending for this population using the 2015 Truven Marketscan claims data (analysis provided by Health Care Markets and Regulation Lab at Harvard Medical School). We inflated those spending numbers to 2019 dollars using actual and projected per capita growth rates for employer-sponsored private health insurance from the CMS Office of the Actuaries.
To construct the consumer portion of premiums, we subtracted the amount that states would contribute toward premiums. The state contribution amount comes from recent estimates from Oliver Wyman of how much federal funds each state would receive out of the Stability Fund. The AHCA allocates $15 billion in 2019 and an additional $8 billion over five years, starting in 2018 — averaging $1.6 billion a year. We adjusted the Oliver Wyman numbers to include the additional $1.6 billion, applying the same allocation distribution to states.
To simplify our computation, we assume that states would apply the entire $16.1 billion (stability funding plus additional appropriation for 2019) to subsidize premiums in state high-risk pools. In states that only use a portion of their allocation to subsidize high-risk pool premiums, consumers would face higher premiums.
We were not able to derive premium estimates for Massachusetts and Vermont because these data were not available from Oliver Wyman. We were not able to derive premium estimates for South Carolina because this data was not available from the Truven Marketscan.




¹ States could qualify for the additional funds if they have a federal waiver that would allow insurers to use health status as a factor in developing premiums.































































