AARP Hearing Center
A Small but Promising Step Toward Better Dental Coverage for People with Medicare
By Claire Noel-Miller, Keith Lind, October 28, 2022 11:42 AM
Note: This blog is an updated version of an October 28, 2022 post. It reflects the new dental health coverage policies in the Centers for Medicare & Medicaid Services’ Calendar Year 2023 Physician Fee Schedule Final Rule.
Medicare is critically important to the health and well-being of millions of older adults and their families. Yet, traditional Medicare, which serves about half the people enrolled in the program, does not cover routine dental care. By law, Medicare does not pay for preventive or diagnostic services such as teeth cleanings or x-rays. It also doesn’t cover basic restorative procedures like fillings or more complex restorative care like dentures or implants—which many older adults need. With very limited exceptions, to get oral health coverage, many people with traditional Medicare pay out-of-pocket or simply forego dental visits. Those who want coverage must buy separate dental insurance (some people with limited resources can get dental coverage through Medicaid). Or they can switch to Medicare’s other coverage option, known as Medicare Advantage, which typically includes limited dental coverage.
A new rule by the Centers for Medicare & Medicaid Services (CMS), which administers the Medicare program, could result in better access to dental coverage for people with Medicare. Here’s a look at what will change and why it is crucial for the program to continue prioritizing improved access to oral care for all Medicare beneficiaries.
How New Rule Will Expand Dental Coverage Under Medicare
Although traditional Medicare doesn’t cover most dental care, the law currently includes an exception for dental services that are necessary to treat an underlying medical condition, under some circumstances (called medically necessary dental care). Historically, CMS has interpreted this exception very narrowly to cover a small number of dental services that are required for the successful treatment of a limited number of medical conditions. Usually, the dental service takes place at the same time or immediately before the covered medical treatment or procedure. For example, Medicare covers dental procedures required as part of jaw reconstruction surgery following an accident, tooth extractions in preparation for radiation treatment for jaw cancer, and oral examinations prior to kidney transplant.
Recently, CMS broadened Medicare beneficiaries’ access to needed dental services by expanding the definition of medically necessary dental care. Although still relatively narrow in scope, the new rule will allow reimbursement for more dental services connected to the treatment of a somewhat broader range of medical conditions than is currently permitted.
Under the new rule, for instance, in addition to reimbursing for oral examinations prior to a kidney transplant, starting in 2023 Medicare will also cover necessary services and supplies (e.g. x-rays, anesthesia, and operating room use) to treat oral infections before such a procedure.
As part of the broader medically necessary dental coverage in 2023 and beyond, Medicare will also cover both oral examinations and other dental services necessary to eliminate an infection for a somewhat larger set of medical conditions—including transplants of organs other than kidneys (for example, liver, bone marrow or stem cell transplants), heart valve repair and replacement, and, starting in 2024, radiation therapies for head and neck cancers. Finally, while CMS did not ultimately include some of the conditions under consideration this year for its expansion of medically necessary dental care, the agency will establish a formal process to consider additional health conditions in the future.
While the expansion of medically necessary dental care does not address older adults’ routine oral care needs, implementing the changes in the new rule will provide critical dental services for some beneficiaries who also need other serious medical or surgical services.
Oral Health Care’s Crucial Role in Health and Well-Being
The evidence is clear: many people with Medicare face significant barriers to accessing the dental care they need. Nearly half of Medicare beneficiaries (47%) do not have dental coverage and are therefore responsible for the entire cost of all routine dental services. As a result, many forego dental care. About 17 million individuals with traditional Medicare (44%) did not see a dentist in the past year.1 Doing without dental care is an issue that disproportionately impacts certain demographic groups within traditional Medicare—including people from Black/African American and Hispanic/Latino communities, beneficiaries with low incomes, and people who live in rural areas (see graphic below).
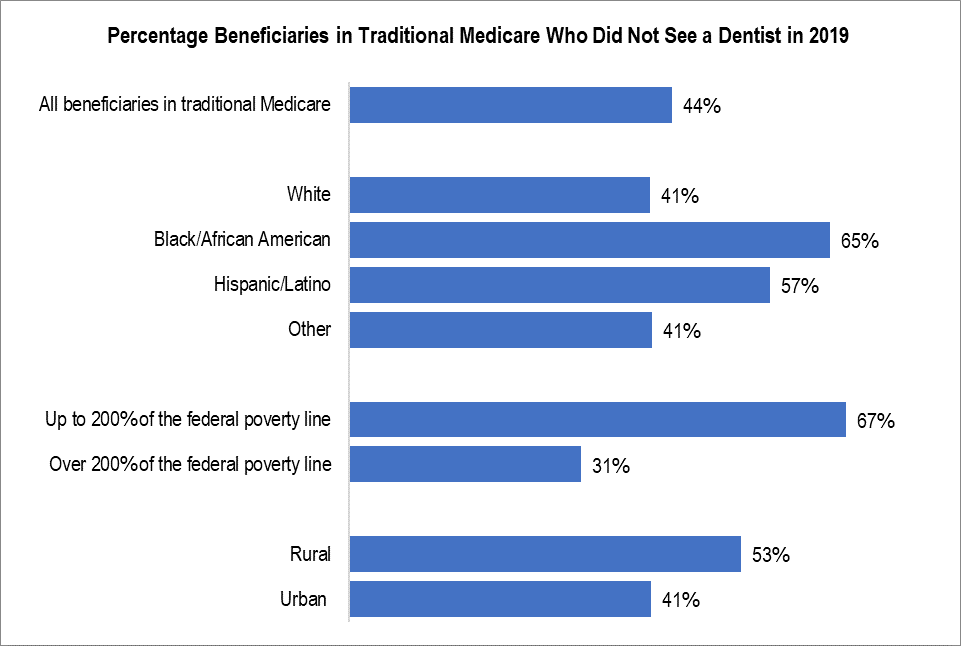
Source: AARP Public Policy Institute’s analysis of the 2019 Medicare Current Beneficiary Survey (MCBS).
And when older adults do get dental care, those services are often expensive. The average person with traditional Medicare who uses dental services spends $940 out-of-pocket each year and one in 10 spends at least $2,135.
Lack of access to dental care can have serious negative implications for older adults’ oral health. According to the Centers for Disease Control and Prevention, one in five adults over 65 have untreated tooth decay, over two-thirds have gum disease, and nearly one in five have lost all their teeth.
Moreover, research shows that poor oral health often has far reaching implications, with potentially dire consequences for people’s overall physical and mental health. For instance, poor oral health among older adults can exacerbate chronic conditions such as heart disease and diabetes, increase the risk of depression and dementia, complicate the treatment of some diseases, and lead to preventable and costly emergency room visits.
Greater Progress Needed
While the new rule is a significant step in the right direction, more should be done. As illustrated above, greater coverage of dental services under traditional Medicare—including routine care—would benefit millions of people and address both oral and medical health needs. Recently, Congress considered but ultimately decided not to add this critically needed benefit to traditional Medicare. Including more comprehensive dental coverage in traditional Medicare would also be valuable to many people with Medicare Advantage, since Medicare Advantage enrollees receive all the benefits available under traditional Medicare.
Although substantially narrower than comprehensive dental coverage, CMS’ new rule to improve medically necessary dental care offers an important opportunity to provide Medicare beneficiaries with more meaningful dental coverage. Fully implementing those changes could mitigate some of the barriers many older adults face when needing dental care to properly treat a serious medical condition. It could also lead to improved health equity as individuals from Black/African American and Hispanic/Latino communities, rural residents, and people with low incomes make up a disproportionate share of beneficiaries with chronic conditions who will likely qualify for expanded medically necessary dental coverage.
Despite its benefits, according to some advocates, the change is still too restrictive. In future rules, CMS should consider expanding medically necessary dental care to include dental services that may not be directly linked to a covered medical procedure but can nevertheless significantly improve the health of people with certain conditions. For example, there is evidence that treatment of gum disease for people with diabetes could lead to both improved patient health and lower health care costs. Another approach is to further broaden medically necessary dental services to include not only dental services that take place before or during a covered medical treatment, but also those that are needed after the procedure (to avoid complications, reduce hospital readmission risks, or improve clinical outcomes, for example).
Beyond medically necessary dental care, policymakers should explore other options to strengthen dental coverage under Medicare. One such option is to launch a limited demonstration to test and evaluate incentives to add routine dental services in Accountable Care Organizations, which serve over 10 million people with traditional Medicare (28%). Other policy initiatives could aim to enhance dental coverage for Medicare Advantage enrollees as those benefits are often limited in scope of services, coverage amount, and provider network.
Looking ahead, it will be critical for Medicare coverage to fully reflect the reality that dental health is an essential part of overall health. To do so, all Medicare beneficiaries should have access to comprehensive, meaningful, and affordable dental coverage.
1 Estimates for the number of people who did not see a dentist and for out-of-pocket spending on dental care are based on AARP Public Policy Institute’s analysis of the 2019 Medicare Current Beneficiary Survey (MCBS).

































































