AARP Hearing Center
The Senate Health Reform Bill Slashes Medicaid in Colorado: State Could Face Cuts Up to $45 Billion
By Susan Reinhard, Ari Houser, Lynda Flowers, Jean Accius, July 13, 2017 02:39 PM
The Better Care Reconciliation Act (BCRA) now under consideration in the Senate would drastically alter Colorado’s Medicaid program. The proposed Senate bill would change the way the federal government currently funds Medicaid by limiting federal funding and shifting cost over time to both states and Medicaid enrollees. The BCRA would subject older adults, adults with disabilities, Medicaid expansion adults, and non-disabled children under age 19 to mandatory per enrollee caps beginning in 2020. State Medicaid programs would have the option to choose between block grants and per enrollee caps for non-elderly, non-disabled, non-expansion adults.
The Senate bill would start out using the medical care component of the Consumer Price Index (M-CPI)—a measure of the average out-of-pocket cost of medical care services used by an average consumer—as the growth rate for per enrollee caps through 2020. Between 2020 and 2024, a growth rate of M-CPI plus one percentage point would be used to trend costs for older adults and adults with disabilities. All other groups would have a growth rate of M-CPI. However, beginning in 2025, the BCRA would slash the growth rate for all populations by switching to the Consumer Price Index for all urban consumers (CPI-U)—a measure of general inflation that examines out-of-pocket household spending on goods and services used for everyday living. Importantly, CPI-U does not tie closely to medical costs—it’s common knowledge that such costs are increasing much faster than general inflation—and will not reflect population growth or the impact of aging. To be clear, none of the proposed growth factors—M-CPI, M-CPI+1, and CPI-U—keep pace with the growth in Medicaid spending. The cut would hit Colorado precisely at the time its aging population will be experiencing additional cost growth due to increasing need for services and supports.
By dramatically reducing the per capita cap growth factor beginning in 2025, we project that the Senate bill would cut between $23 billion and $45 billion from total (federal and state) Medicaid spending in Colorado over the 20-year period between 2017 and 2036 for the four non-expansion Medicaid enrollment groups: older adults, adults with disabilities, non-disabled children under age 19, and non-expansion adults (children with disabilities are excluded because the BCRA does not subject them to capped funding). A cut of this magnitude threatens the viability of Colorado’s Medicaid program in unprecedented ways and will likely increase the number of people who no longer have access to essential healthcare services and critical supports. The projections do not include the proposed cuts to the adult expansion population, which would also be considerable for the state of Colorado.
Previous analysis by the AARP Public Policy Institute discusses why capping Medicaid is flawed and would leave states—and the poorest and sickest Americans—holding the bag for the shortfalls that will most certainly occur.
Table 1 shows the cumulative 20-year cuts to Medicaid by eligibility group in Colorado under the Senate health reform bill for three growth rate projections. The bill would cap per enrollee cost growth using two measures of inflation (M-CPI and CPI-U), which are highly variable and uncertain, though will fall well short of what is needed to maintain the integrity of Colorado’s Medicaid program. It is difficult to plan for such uncertain growth rates, and reasonable projections are far apart.
We present the high, middle, and low case for M-CPI/CPI-U growth rates based on the following:
- Low Case. Based on historical growth rates. Over the last five years (2012-2016), the M-CPI growth rate has averaged 3.0% per year, and the CPI-U growth rate has averaged 1.32% per year.
- Middle Case. Based on projections from the Congressional Budget Office. CBO projects M-CPI to grow by 3.7% per year, and CPI-U by 2.4% per year.
- High Case. Based on projections from 2016 CMS Medicaid Actuarial Report. From 2019 onward, this report projects M-CPI to grow by 4.2% per year, and CPI-U by 2.6% per year.
In short, the lower the cap growth rate, the more severe the Medicaid cuts will be.
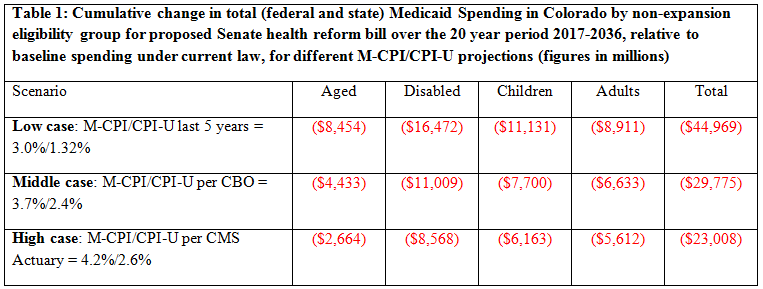
Table 1 above demonstrates that for any projection of the bill’s cap growth rates, the BCRA will lead to significant funding shortfalls for older adults, adults with disabilities, and non-disabled low-income children under age 19 in Colorado. The end result is that the state will be left with severe funding shortages, forcing Colorado to cut eligibility, provider rates, or covered services—or very likely all three. Moreover, many of Colorado’s most vulnerable citizens will be left without access to the critical health care and long-term services and supports—like help with toileting, bathing, dressing, and eating—they rely on. Cutting between $23 billion and $45 billion from Colorado’s Medicaid program is not the way to go.

Susan Reinhard is a senior vice president at AARP, directing its Public Policy Institute, the focal point for AARP’s public policy research and analysis. She also serves as the chief strategist for the Center to Champion Nursing in America, a resource center to ensure the nation has the nurses it needs.

Jean Accius is vice president of livable communities and long-term services and supports for the AARP Public Policy Institute. He works on Medicaid and long-term care issues.

Lynda Flowers is a Senior Strategic Policy Adviser with the AARP Public Policy Institute, specializing in Medicaid issues, health disparities and public health.

Ari Houser is a Senior Methods Adviser at AARP Public Policy Institute. His work focuses on demographics, disability, family caregiving, and long-term services and supports (LTSS).































































