AARP Hearing Center
Medicare Spending Is Growing Slower Than Expected
By Keith Lind, Harriet Komisar, April 24, 2023 11:36 AM

Medicare spending growth rates in the decade before the pandemic were substantially lower than expected, according to a recent analysis by the U.S. Congressional Budget Office (CBO). In addition, both CBO and a new report from the Medicare Trustees forecast that Medicare spending growth in the upcoming decade will also be lower than previously expected. These trends mean that people with Medicare, as well as the federal government, are seeing significantly lower costs for Medicare than had been expected.
CBO’s analysis
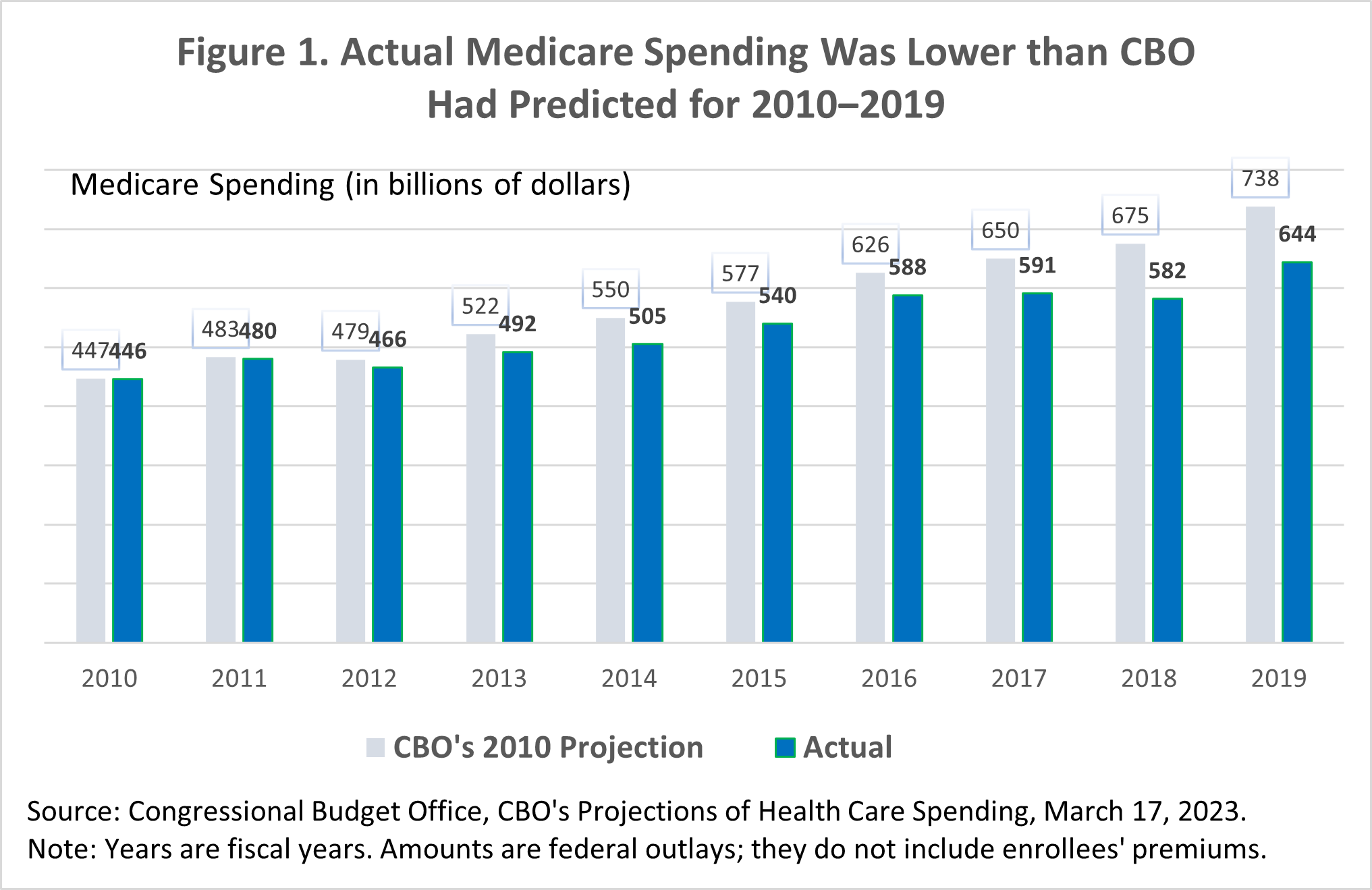
When CBO compared its 2010 estimates of future Medicare spending with what actually occurred, the findings proved revealing. Between 2010 and 2019—the decade before the COVID-19 pandemic—Medicare spending was 7 percent lower than CBO had predicted in 2010. The federal government spent $413 billion less for Medicare from 2010 through 2019 than CBO had expected (see Figure 1).
Spending in 2020‒2022, during the pandemic, was also lower than CBO’s earlier estimates. And CBO’s current forecast for the upcoming decade (2023‒2032) predicts slower Medicare spending than CBO’s earlier projections.
What drove the spending trend
According to CBO’s analysis, the lower spending in the 2010‒2019 period was primarily due to an unexpected decline in spending per person enrolled in Medicare, rather than to policy changes or discrepancies between the projected and actual number of Medicare enrollees.
This is part of a decreasing cost trend that began before the COVID-19 pandemic. Medicare’s average yearly rate of growth in spending per person fell from an average of 6.6% per year from 1987–2005 to 2.2% per year from 2013–2019, or by 4.4 percentage points (see Figure 2). When we adjusted for inflation, the 2013‒2019 growth in spending per enrollee averaged only 0.6% per year. And during the most recent three years, from 2020 through 2022, inflation-adjusted spending per enrollee actually fell by about 1.2 percent per year, according to our estimates.
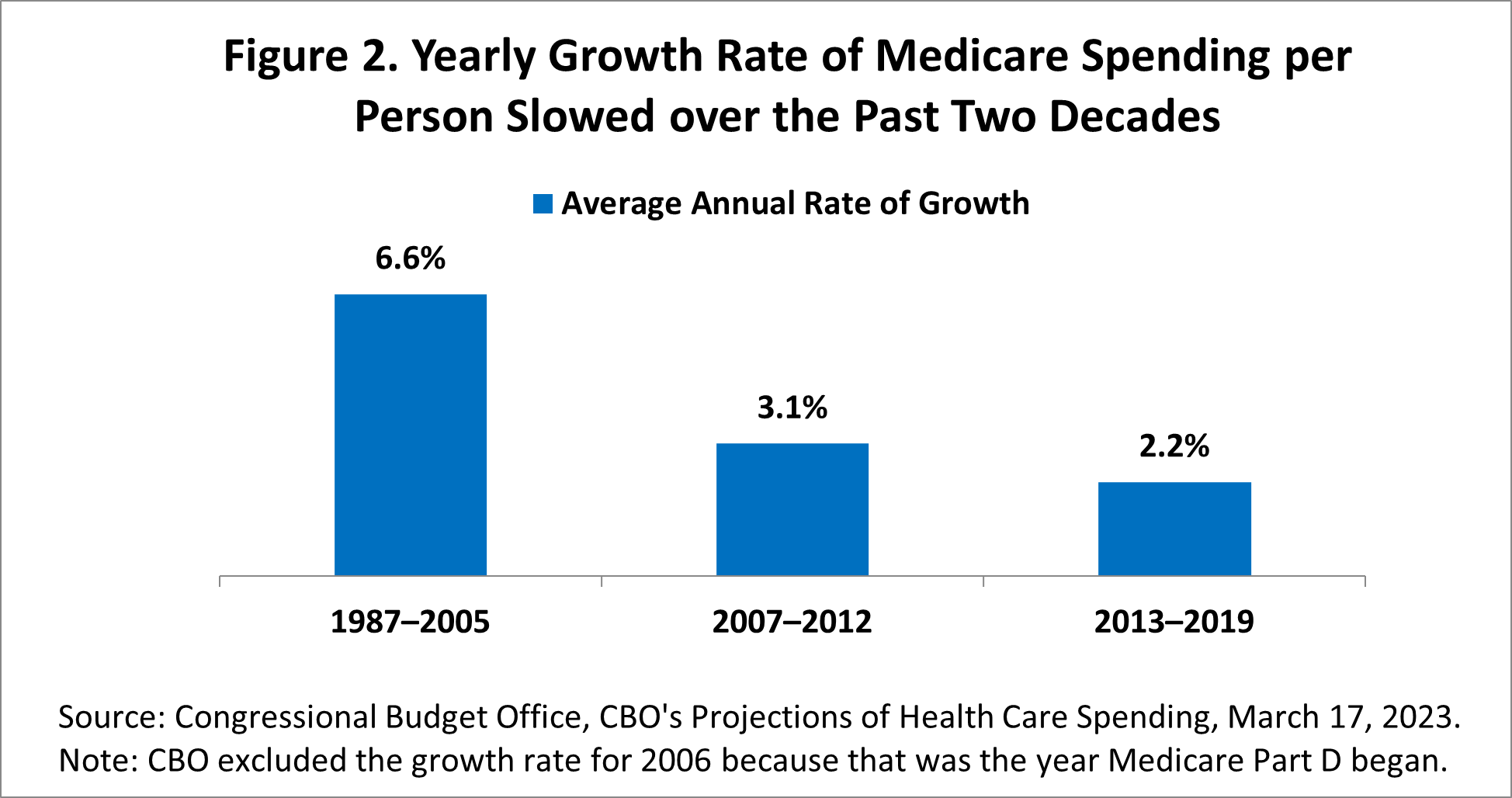
CBO attributed much of the difference between its predictions and what actually occurred from 2010 to 2019 to lower spending on Medicare Part D prescription drugs. One important source of these savings was greater use of generic drugs, which became more widely available as expensive brand-name medications lost their patent protection.
The slowdown in Medicare spending per person also reflects decreases in spending for people with cardiovascular disease, thanks to better management of conditions, such as hypertension and diabetes, that are risk factors. In addition, CBO found that slower spread of expensive new technologies and slower growth of Medicare provider payment rates contributed to the lower-than-expected spending.
Savings for people with Medicare
The decline in Medicare spending means those enrolled in Medicare have been spending less on Medicare premiums and cost sharing than they otherwise would have if actual spending had tracked with the 2010 projections.
Looking ahead
In another recent report, the Medicare Trustees also project slower growth in Medicare spending for the next decade than previously expected. The report attributes the slower growth to a complex mix of reasons, including pandemic-related deaths that both decreased the number of people with Medicare and led, on average, to a healthier Medicare population than previously expected. Other factors include policy changes and the shift of some joint replacement surgeries from hospital inpatient to outpatient settings.
Slower growth will help strengthen Medicare’s overall financial outlook. It will also help extend the solvency of Medicare’s Part A Trust Fund, now estimated by the Trustees to remain solvent until 2031—three years longer than last year’s Trustees’ report had forecast (because of both lower spending and higher revenue from payroll taxes than predicted last year). Slower growth will also mean continued lower increases in premiums and cost sharing for people with Medicare.
There are many policies and policy proposals that could help ensure that Medicare spending remains lower than expected in the future. For example, Medicare spending will slow as the prescription drug provisions of the Inflation Reduction Act are implemented. Additional savings could come from strengthening and expanding promising innovative models that deliver person-centered care. These and other improvements could help improve program efficiency, clinical outcomes, and quality of care, while continuing to slow the growth in spending.

































































