AARP Hearing Center
Telehealth and Medicare: The Use of Audio-Only Visits
By Harriet Komisar, August 3, 2023 10:09 AM

During the COVID-19 pandemic, telehealth visits became a vital part of health care for Americans of all ages. Telehealth visits are medical care appointments conducted remotely by video or telephone rather than in-person in a doctor’s office or other traditional setting. In 2020, about 40% of people with Medicare used telehealth visits—up from fewer than 1% in 2019, before the pandemic. And in 2021, even as Medicare enrollees returned to using more in-person visits, still more than one-fourth used telehealth visits.
The quick adoption of telehealth was made possible because Medicare expanded its coverage of these visits during the COVID-19 public health emergency to allow people with Medicare to participate in telehealth visits for a wide range of services from their home. In contrast, before this expansion, Medicare coverage of telehealth was much more limited and did not cover telehealth visits in a person’s home. Most of the coverage expansions are temporary, however, and scheduled to expire at the end of 2024. An exception is mental health services, for which most telehealth expansions are now permanent. While many people expect telehealth to be part of their health care in the future, Medicare telehealth coverage for most services is not assured.
One of the key decisions facing lawmakers is whether Medicare will continue to cover audio-only (that is, telephone-without-video) visits. A different option is to require telehealth to use communication platforms that include a visual component and no longer cover audio-only visits. That would represent a major change from current Medicare telehealth coverage under the temporary expansion, and one with potentially significant implications.
The role of audio-only visits
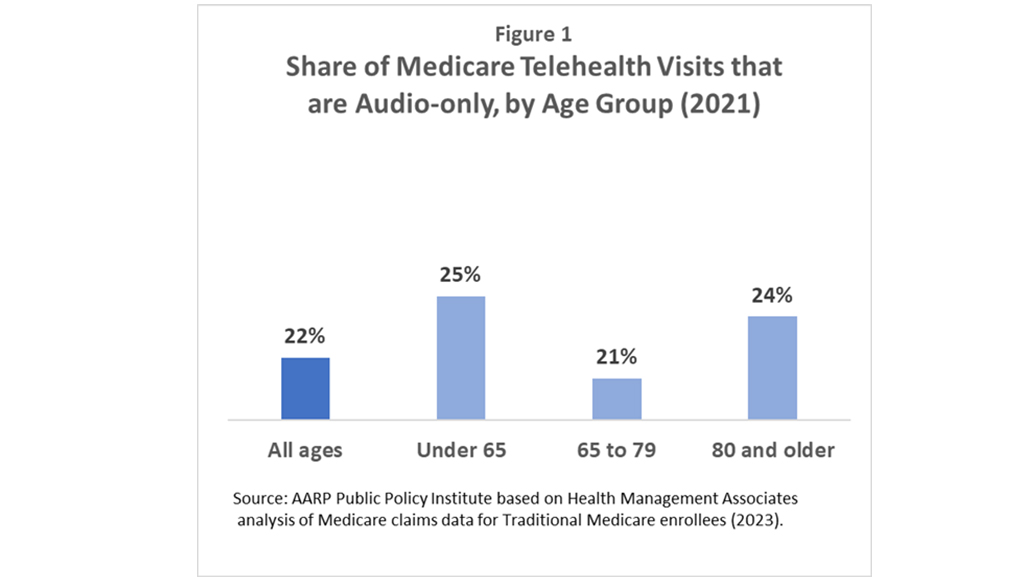
Audio-only telehealth visits play a large role in delivering telehealth services. In 2021, more than one in five Medicare telehealth visits was an audio-only visit (see Figure 1). Audio-only visits served an even larger role for Medicare enrollees aged 80 or older, as well as for those under age 65 who are eligible for Medicare because of long-term disabilities. Among enrollees aged 80 and older, 24% of telehealth visits in 2021 were audio-only. Similarly, among enrollees under age 65, 25% of telehealth visits were audio-only.
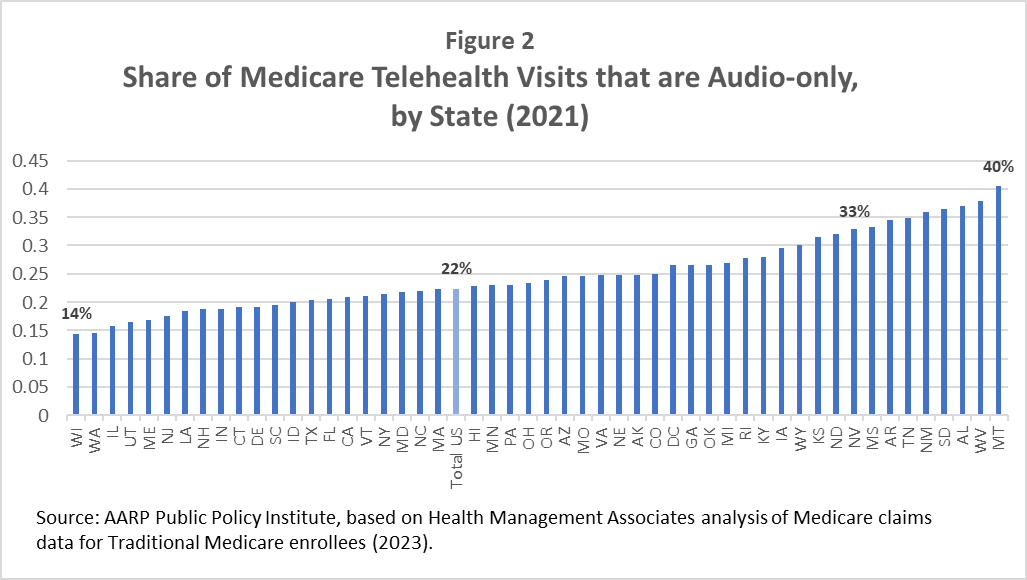
The use of audio-only visits also varies among states. In 2021, the share of Medicare telehealth visits that were audio-only visits ranged from 14% to 40% among states (see Figure 2). In nine states, 33% or more of Medicare telehealth visits were audio-only.
Audio-only visits can enhance access to care
For some individuals, audio-only visits may be their only telehealth option because they don’t have access to the equipment or internet service needed for audio-visual visits. Others may have difficulty using video visits—whether because of health conditions, limited experience with video platforms, or other factors—or may prefer not to use them for various reasons. For example, some individuals may not trust video platforms or may be uncomfortable with a visual component to a telehealth visit because of privacy concerns.
Barriers to audio-visual telehealth are even more common among older people, people with lower incomes, and people living in rural areas. Barriers include less access to the internet and to computers and smartphones. For example, in 2020, Medicare enrollees living in rural areas had lower rates of internet access than urban enrollees (78% versus 84%) and of owning computers (58% versus 66%) or smartphones (60% versus 72%).
Importantly, research also has revealed that the availability of audio-only visits not only enhances access to telehealth, but also enhances access to any type of care. By offering audio-only appointments, community health centers reduced “no-show” rates, improved providers’ relationships with their patients, and were able to treat a larger number of people with chronic conditions or behavioral health care needs, the research found.
Audio-only telehealth visits: concerns could be addressed while maintaining coverage
Some experts have questioned whether Medicare should continue to cover audio-only visits. In addition to questioning the quality of audio-only visits, they cite concerns that such visits may be used more frequently than actually needed, running up Medicare costs, and that there could be a higher risk of fraud than with audio-visual telehealth visits.
However, concerns about audio-only visits could be addressed in other ways. For example, Medicare could enhance its methods for identifying fraudulent telehealth claims. Another option is to limit coverage of audio-only visits to individuals who are not able to access telehealth using audio-visual communication methods, similar to the approach Congress adopted in permanently expanding Medicare coverage of telehealth for mental health services after the public health emergency.
Looking ahead
Within less than two years, Congress must decide whether Medicare coverage will continue to include audio-only telehealth appointments after 2024, as well as the extent to which Medicare will continue to cover telehealth visits in general. The experience of the past few years has demonstrated that telehealth—including audio-only visits—is widely used by Medicare enrollees.
In the future, audio-only visits will likely remain a preferred—or only feasible—form of telehealth for millions of people with Medicare. Given this reality, Congress should carefully consider the potential health and access implications of continuing to allow Medicare coverage of audio-only appointments.
































































